Alzheimer’s disease (AD) is a progressive neurodegenerative disorder characterized by cognitive decline, memory loss, and impaired daily functioning. According to the National Institute on Aging, it currently ranks as the seventh leading cause of death in the United States. Alzheimer’s is also a major public health challenge affecting millions worldwide. Combating Alzheimer’s is crucial and top of mind for scientists across the globe.
The Alzheimer’s Association states that Alzheimer’s is the most common cause of dementia, accounting for approximately 60-80% of all cases. The disease causes individuals to lose their identity, sense of self, independence and eventually, their lives. Alzheimer’s impacts family caregivers too, causing many to sacrifice their health, personal relationships and careers.
This type of dementia brings significant financial burdens to patients, families and our communities. A recently released Alzheimer’s Facts and Figures report estimates that in 2023, caring for individuals with Alzheimer’s disease comes at a cost of $345 billion.
Alzheimer’s Risk Factors

A person’s risk of developing Alzheimer’s increases with age. The vast majority of cases occur in older adults who are over 65 years of age. Other factors known or believed to increase the risk of developing Alzheimer’s disease include:
- Genetic predisposition
- Family history of the disease
- Vascular conditions
- Depression
- Lifestyle habits including diet, exercise, and smoking
- Down Syndrome
- Head injuries and past head trauma
- Brain health
- Ability and desire to remain socially active
We are unsure of the cause of this disease. However, we do know that amyloid beta plaques (Aβ) are connected to the development and progression of Alzheimer’s. Scientists are studying this form of dementia and working on new therapies to reduce Aβ plaques. The hope is that medications might slow down or even halt the progression of Alzheimer’s disease.
To better understand the scientific community’s views on Alzheimer’s disease, let’s explore Aβ plaques and their connection to this dementia. Later, this blog will highlight several newly developed medications that show potential for treating Alzheimer’s.
Amyloid Beta Plaques
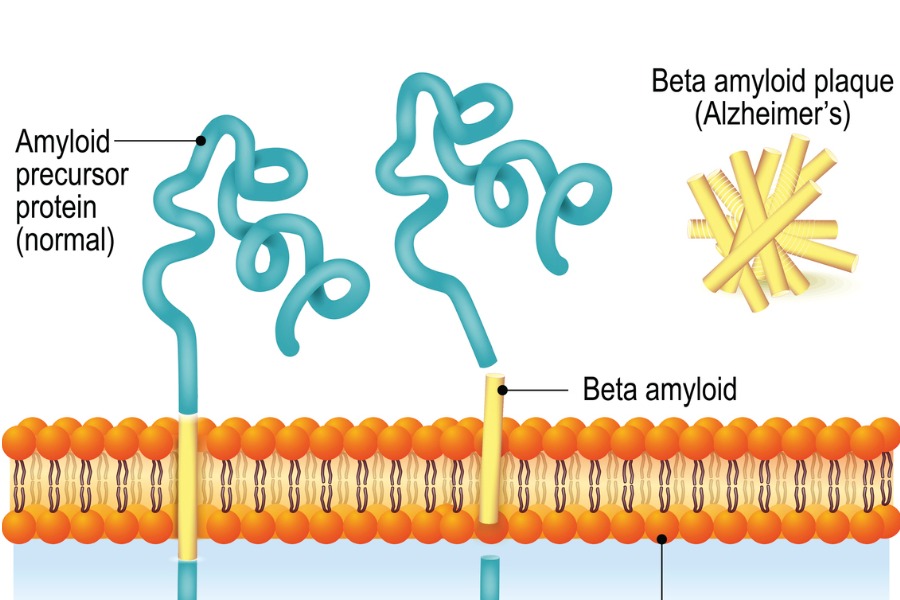
The hallmark pathological feature of Alzheimer’s disease is the accumulation of amyloid beta (Aβ) plaques in the brain. To better understand what scientists know about Aβ, we must first understand amyloid-beta precursor proteins.
The amyloid-beta precursor protein (APP) is an integral membrane protein. It exists in all humans’ bodies. APP plays an important role in the growth and repair of brain cells and cell adhesion.
When broken down, smaller elements of this protein include amyloid beta plaques. Healthy individuals efficiently clear Aβ from the brain. However, in Alzheimer’s disease patients, an imbalance between production and clearance leads to the aggregation of Aβ into insoluble plaques. These plaques are neurotoxic and disrupt normal brain function, contributing to the neuronal death and cognitive decline observed in Alzheimer’s patients.
Despite significant efforts to develop effective treatments, there is currently no cure for AD. However, emerging research into new medications targeting Aβ plaques offers hope for improved disease management and potentially even disease-modifying therapies.
New Medications Targeting Aβ Plaques:

Several Alzheimer’s medications are currently available or in various stages of clinical trial and development. Some treatments have shown potential in targeting Aβ plaques and changing the progression of Alzheimer’s disease to enhance quality of life.
For many of these medications, the goal is to slow cognitive decline. This offers significant benefits including potentially preventing aging individuals from entering late-stage Alzheimer’s in their lifetime. A few current options include:
a. Anti-Amyloid Antibodies: Monoclonal antibodies that specifically target Aβ have garnered significant attention. These antibodies can bind to Aβ plaques, promoting their clearance and reducing their toxic effects. Promising clinical trials have occurred or are currently underway. They showed that certain antibodies can reduce Aβ plaques and slow cognitive decline in people with AD.
b. BACE Inhibitors: These medications target an enzyme that starts the process of forming plaques in the brain. By blocking this enzyme, they can potentially slow down the production of plaques and slow the progression of Alzheimer’s disease. Several BACE inhibitors have reached clinical trials. While some have shown promising results, they have also encountered various challenges related to safety and efficacy.
c. Gamma-Secretase Modulators: Gamma-secretase plays a role in the final cleavage of APP to generate Aβ. Gamma-secretase modulators aim to selectively influence the production of less toxic forms of Aβ, reducing the aggregation of plaques. Clinical trials investigating these modulators are ongoing, and results for some are promising.
d. Aβ Immunotherapies: Scientists are studying ways to treat Aβ, such as vaccines or transferring immune cells that target Aβ. They are also researching monoclonal antibodies, created by cloning a unique parent white blood cell, as a potential treatment for Aβ. Immunotherapies such as Donanemab hold promise as they might stimulate the body’s immune response to clear Aβ plaques actively.
This is by no means an exhaustive list of all treatment options. The scientific community continues to research and learn more about Alzheimer’s. This new knowledge leads to the refinement of existing therapies and exploration of potential medications and therapies.
Challenges and Future Direction

While the development of medications targeting Aβ plaques is encouraging, challenges remain in the search for effective Alzheimer’s treatments. Clinical trials have faced issues related to patient selection, common side effects, dosing, and trial design. Alzheimer’s disease is also complex and involves other factors including tau protein tangles. Therefore, effective care and treatment requires a multifaceted approach that includes both pharmaceutical and non-pharmacological treatments (NPT).
Future research needs to focus on combination therapies that address multiple aspects of the disease. Scientists also understand the benefits of identifying AD biomarkers while studying bodily fluids of patients with Alzheimer’s. This discovery enables early diagnosis and empowers individuals to begin treatment in the earliest stages of the disease. Early diagnosis provides more treatment options for the patient with Alzheimer’s.
Additionally, ongoing efforts to improve drug delivery systems and address potential safety concerns are crucial for successful drug development. These include reducing opportunities for misdosing or overdosing. Current options include offering extended release medications, intranasal administration of medications, and nanotechnology delivery systems, among others.
Summary

Alzheimer’s is a debilitative disease that impacts quality of life for millions of Americans. The cost of caring for individuals with Alzheimer’s is also staggering.
We do not fully understand this form of dementia. However, the build-up of amyloid beta plaques is a significant contributing factor. Targeting these plaques with new medications holds significant promise for disease management. They are most effective when combined with NPT, through a multifaceted approach.
With care and support, we aim to improve the quality of life and promote healthy aging for people with Alzheimer’s.
While challenges persist, ongoing research into anti-Aβ therapies offers hope for the future. With time and study, researchers may discover effective treatments for Alzheimer’s disease. The potential exists to delay the progression of mild or moderate Alzheimer’s disease. Perhaps, in the future, we might even see a cure developed.
Continued dedication to understanding AD pathophysiology and developing innovative treatments is vital in the quest to conquer this disease. Ultimately, doing so will improve quality of life and promote healthy longevity for persons with Alzheimer’s disease.
Salus Dementia Care Programs

Salus remains abreast of the latest senior care innovations coming out of the scientific community. We support endeavors to combat Alzheimer’s with medications and other therapies. As new information emerges, we strive to share it with our professional team, patients and their family members.
While we wait for advancements in dementia treatment or even a cure, support remains available for older individuals with Alzheimer’s.
Salus Homecare is here to help. We offer a continuum of care that includes a range of home care, home health and hospice care services. Our goal is to help you and your loved one better cope with Alzheimer’s disease and improve quality of life.
Senior care professionals highly recommend us. Our services also receive 5-star ratings from patients and families, and we hold Joint Commission accreditation. This is our assurance to you that choosing Salus means choosing the very best professional care for your loved one.
Contact us today to learn more or schedule your free, no obligation consultation.

